|
We’ve all had our tire pressure light come on our dashboard before. If you’re like me, you know you should go get it checked before getting on the freeway, but you likely put it off, brushing it off as a change in temperature or a faulty sensor. Oftentimes it’s a quick fix for a minor loss of tire pressure, and you’re back on your way again after taking the time to have your tire checked. But what if you kept putting it off, letting the tire continue to lose air, and ultimately putting yourself at risk for a much bigger problem?
A common complaint I hear from people considering whether to pursue treatment for their jaw is, “It bothers me sometimes, but not all the time.” Or, “It pops and clicks, but it doesn’t really hurt.” After answering a few more questions about their jaw and daily life, they often remember that they actually do have more specific issues related to their jaw that are quite bothersome. Whether you’re having trouble opening wide for long periods at the dentist (or opening at all), or notice popping and clicking when you’re eating, these are your jaw’s warning signs lighting up on your body’s dashboard. The longer you delay getting treatment for these problems, the greater the risk for developing more complications within the jaw joint, and the chance of achieving long-term resolution of your symptoms with conservative treatment decreases. If you notice something isn’t right, don’t wait until you are in pain to seek help. Clicking and popping are warning signals of deeper issues, and physical therapy helps. Check out our Getting Started section to learn more about how you can get ahead of your jaw, neck, or head pain. Caitlin Ayres, PT, DPT, CFC
2 Comments
What is dry needling?
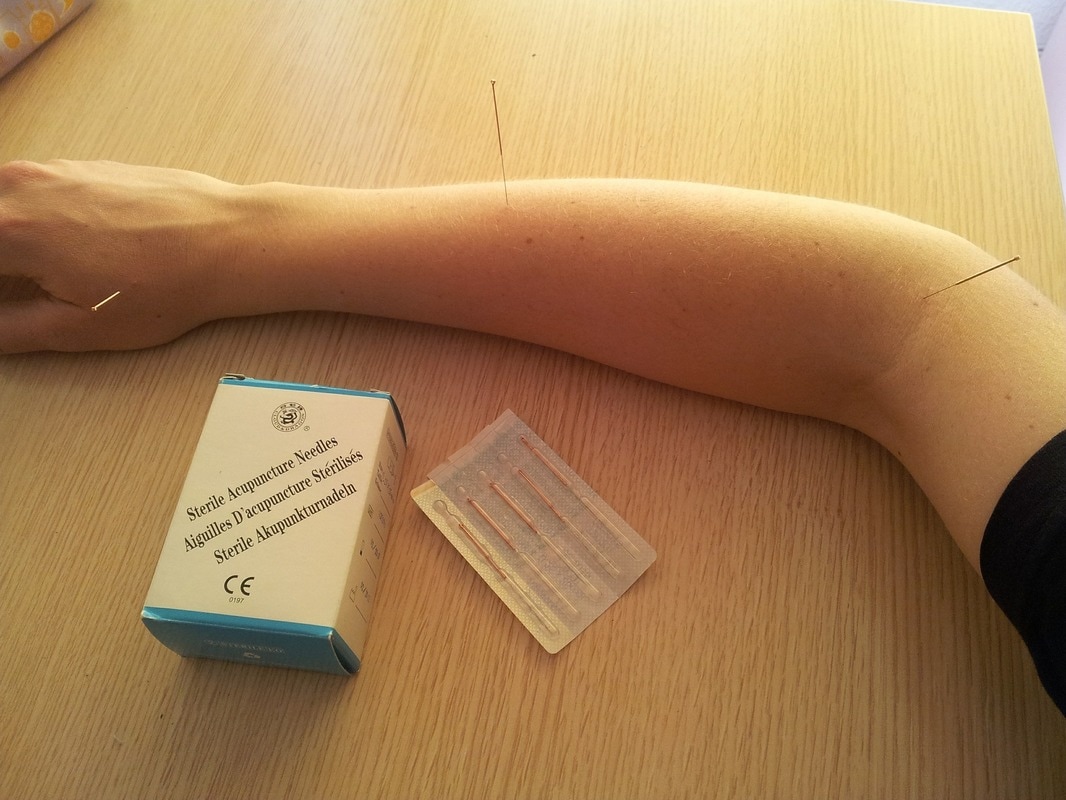
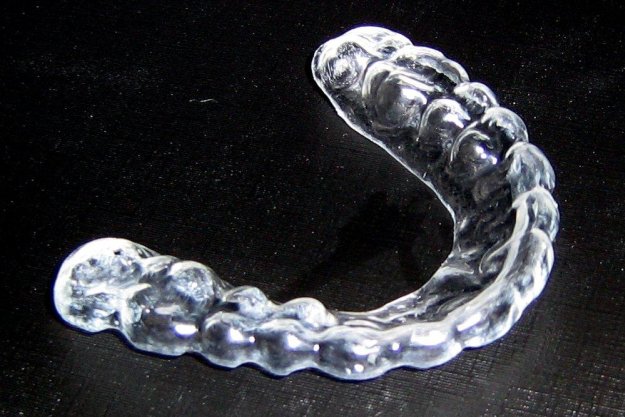
Dry needling is gaining momentum in the physical therapy community as an adjunct treatment for myofascial pain, or pain stemming from a “trigger point” in a muscle. We have trigger points in lots of places, but in folks with chronic neck pain, headaches, or jaw pain, there are a specific few that a trained practitioner can target in treatment. There is a difference, however, in “latent” trigger points, non-tender taut bands of tissue, and “active” trigger points, taut bands of tissue that when touched by either you or your physical therapist, you say, “Ow! Yep, that’s it!” You can sometimes pinpoint exactly where your pain is in a muscle, and in these cases dry needling can help. Not all physical therapists offer dry needling, as it requires additional post-doctoral training to acquire this specific skill set. HCHN is proud to offer dry needling to patients following Dr. Ayres' training with the Spinal Manipulation Institute. How does it work? We use a sterile, thin, filiform needle, and insert it into the trigger point. This creates a small muscle spasm in the trigger point by disrupting the neuromuscular junction. Thus, bloodflow is stimulated within the muscle group to clear out the metabolic waste products and initiate the healing process, and the muscle relaxes in response to the needle. Patients often notice a difference in their pain and symptoms as well as their range of motion very quickly following dry needling. Does it hurt? In short, no. Your physical therapist will feel in the muscle to find the trigger point before inserting the needle, and oftentimes this is the most uncomfortable part of the treatment. The needle insertion is quick and somewhat surprising, but not painful. Sometimes, patients cannot even feel the needle go in. There is a deep ache in the muscle once the trigger point is targeted by the needle, but the ache will dissipate over the course of several minutes. There may be some minimal soreness following the treatment, but it should go away within 48 hours. This is normal, as the healing response is taking place inside a muscle that previously was not getting enough bloodflow. What kinds of conditions can be treated with dry needling? While trained physical therapists can treat painful muscles all over the body with dry needling, HCHN focuses on muscle groups in the head, neck, face, and upper back. Muscles in the neck and face can contribute to chronic headache, TMJ pain, and neck pain, to name just a few of the more common conditions we treat. If you have questions about if dry needling can help a specific painful area, email us and we can talk more about it! For more information, check out this website. It has a great explanation of dry needling in physical therapy, as well as a video that shows a dry needling treatment. Most of the time, if you visit your dentist and tell him you're experiencing TMJD symptoms, he will suggest fitting you for an occlusal guard, also known as a bite splint or a night splint. This serves several purposes - protecting your teeth and gums from the wear and tear caused by grinding or clenching during your sleep, helping to optimally reposition the jaw joint, muscle relaxation, and altering the inputs the muscles and joint receptors in the TMJ provide to the brain, which ultimately can lead to an inhibited reflex from the trigeminal nucleus in the pons medulla, AKA less pain!1
But is that enough to promise relief from the clicking, popping, pain, headaches, and limitation in movement? Studies on the efficacy of splints alone in treating TMJ dysfunction are inconclusive.2 This does not mean that they do not serve a purpose or just plain don’t work, but it does mean that there are other non-invasive treatments (like physical therapy!) that may help in conjunction with the right splint. Your physical therapist can help make sure your horizontal occlusal plane (read: the way you bite and where you contact first with your teeth) is level through addressing postural and mechanical problems, aid in relaxing areas in your head, face, and jaw muscles that are painful from overuse even at rest, and work with your dentist to make sure your splint is appropriate for the changes your bite may undergo during treatment. The right combination of treatments is an effective and cost-efficient approach to making sure your jaw is stable and able to function properly while you bite, chew, smile, yawn, and sleep. Unsure if your splint is doing enough to get you relief? Ask your dentist to refer you to HouseCall Head and Neck for physical therapy, it may be the smartest health move you’ll make! 1. Okeson, J. 2013. Management of Temporomandibular Disorders and Occlusion. 7th Edition. 2. Dao, TT; Lavigne, GJ. “Oral splints: the crutches for temporomandibular disorders and bruxism?” Critical Review of Oral and Biological Medicine. 1998; 9:345-361. (Image courtesy of http://teethgrindingsupport.com/clenching-teeth-jaw-use-mouth-guard-clenching/) Happy TMJ Awareness Month! Fall is notorious for jaw pain, and the culprits are all things you’ve likely eaten this season. Now you probably won’t be eating pumpkin quite like this guy, but here are a few things you might want to think twice about putting on your plate this Thanksgiving if you have popping, clicking, or pain with chewing or opening your mouth:
-Corn on the cob -Candy apples -Whole apples -Peanut brittle -Nuts -Taffy -Caramel -Tough, thick cuts of meat -Raw carrots -Celery Repetitive motions such as prolonged chewing (think chewing gum) can fatigue the jaw through unnecessary stress put on the TMJ muscles and ligaments. Similarly, opening too wide to bite into an apple or corn on the cob can lead to not only pain, but sometimes even what we call an acute closed-lock, or lockjaw. The best way to combat jaw pain during your holiday parties is to pick softer foods or cut up food into smaller, more manageable bites. Sweet potatoes, tender cuts of turkey, cranberry sauce, and pumpkin pie are all TMJ-friendly foods, and are good for you, too! If you do start to experience a sudden, sharp onset of jaw pain or difficulty opening your mouth, visit your dentist as soon as you can. They may be able to prescribe some medications to help with the discomfort, and they may also refer you to physical therapy to help regain any lost motion and help stabilize your jaw so you are able to enjoy your favorite holiday foods without pain or limitation. Don’t wait for your dentist to refer, ASK for a physical therapy referral! Patients who receive physical therapy from a trained craniofacial PT in conjunction with dental interventions get better faster and more completely than those who only have dental treatment. Take this referral form with you when you go. We have so much to be thankful for at HouseCall Head and Neck, and wish you and your family a Happy Thanksgiving full of love and gratitude. For as many people as there are who suffer from jaw pain, very few know that physical therapy can help alleviate their symptoms, and even fewer understand how it can help. I'm here to answer some frequently asked questions about physical therapy for the TMJ, and inspire hope in those who feel like they've tried everything and are still suffering. This is the first post in a series of posts, so keep a lookout on our Facebook page for updates. And while you're there, give us a like if you haven't yet!
"So, how does physical therapy work for the jaw?" I'm asked this question a lot! Physical therapists who are trained to treat patients with jaw (or TMJ) pain focus on the big picture in what is causing the dysfunction. The TMJ (short for temporomandibular joint) is controlled by muscles in the face and neck, and when these muscles don't function properly, it can lead to poor movement patterns which can cause painful clicking, popping, and locking in the joint. While patients often come to me with a primary complaint of pain in their jaw or face, the underlying issue is almost always their posture. Sometimes patients recall having pain in their neck or head when asked, but others forget even having pain until I bring it up! On the first visit, I perform a thorough examination of the cervical spine, face, and jaw, and assess movement and posture. This gives me an idea of what factors are at play in the mobility of the TMJ. From there, I implement manual therapy techniques to help relax muscles and improve mobility in areas that are stiff, and also teach my patients specific exercises to help alleviate their pain and improve function between treatment sessions. Other important components to therapy treatments include muscle relaxation techniques, and neuromuscular re-education to retrain muscles to function properly, identifying habits that are detrimental to daily function, stress management solutions, and lifestyle modification. "I wake up with headaches, my jaw hurts, and sometimes even pops and clicks when I open my mouth too far. Can I come to you for treatment?" Absolutely! Before we get started, be sure to ask for a referral for physical therapy from your dentist, physician, or nurse practitioner. There are a few other providers who can refer you, too. When you ask them, take this form with you and have them fill it out, then email it before your first visit or have it handy at your initial evaluation. Also, check out our Getting Started page, and fill out those forms beforehand. After that, we can start getting you back to your personal pain-free best! |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
March 2018
Categories |

 RSS Feed
RSS Feed